What is Bronchiectasis?
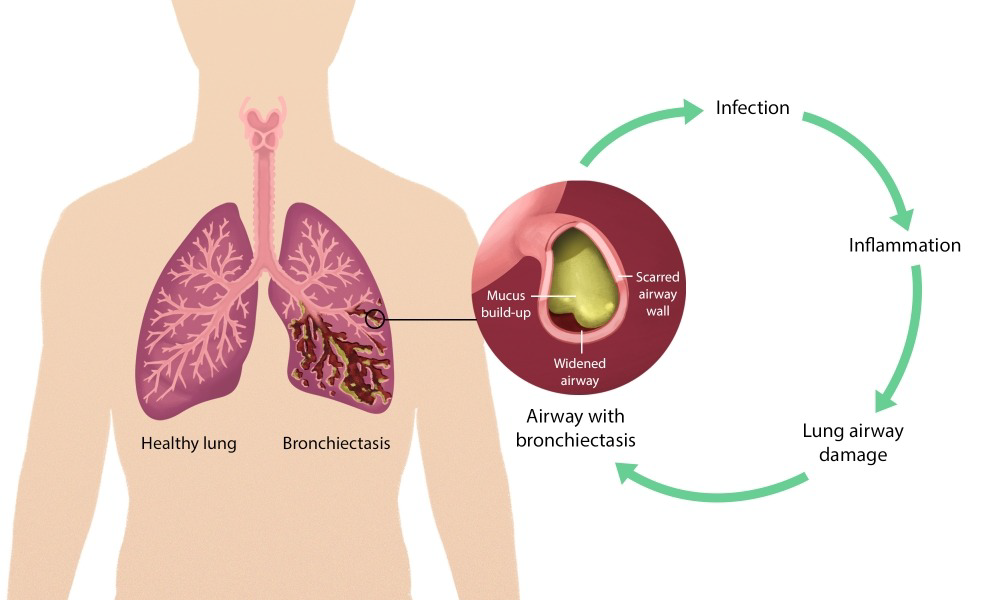
Bronchiectasis (bron-kee-eck-tuh-sis) is a condition affecting the airways in the lungs that causes cough, increased mucus production, and recurrent lung infections. The symptoms are caused by abnormal widening of the airways of the lung, also known as bronchi. The cells lining the airways become inflamed and swollen. These damaged airways can no longer effectively clear mucus and bacteria from the lung. This can lead to flare-ups of cough, mucus production, and shortness of breath.
Understanding the Vicious Vortex of Bronchiectasis
Bronchiectasis is caused by one or more infections introduced into the lungs. People with bronchiectasis are more likely to get lung infections. Each lung infection can make the bronchiectasis worse. Therefore, early diagnosis and treatment of bronchiectasis is very important.
Signs & Symptoms of Bronchiectasis
Often developing gradually, symptoms of bronchiectasis may not appear for months or even years after the pre-disposing event or events. Some of the signs and symptoms of a bronchiectasis exacerbation are the same as those of acute Bronchitis and COPD making them hard to differentiate.

Bronchiectasis can be tricky because it often presents like Chronic Obstructive Pulmonary Disease (COPD), but won’t respond to COPD therapy. In fact, studies show it’s much more prevalent than what’s being diagnosed.
Studies show almost 1 in 2 COPD patients may have bronchiectasis,1 70,000 new patients each year2
Patients suffering from:
- Long-term productive cough
- Recurring chest infections
- Frequent exacerbations requiring antibiotics, i.e., recurring pneumonia
- Frequent hospitalizations
…should be screened for bronchiectasis.
Airway Clearance Therapy for Bronchiectasis
A well-rounded treatment plan incorporating antibiotics, periodic testing and airway clearance helps manage the symptoms of this chronic disease.
Airway Clearance Therapy (ACT) is considered the cornerstone of therapy aimed at minimizing the effects of airway obstruction, infection, and inflammation in lung diseases such as bronchiectasis.
1. Kosmas E, et al., Bronchiectasis in Patients with COPD: An Irrelevant Imaging Finding or a Clinically Important Phenotype? CHEST 2016;150(4):894A.
2. Weycker D, et al., Prevalence and Incidence of Non-cystic Fibrosis BE Among US Adults in 2013. Chron Respir Dis 2017. Nov;14(4): 377-384.